Mouth cancer survival
Overall, there have been modest improvements in mouth cancer survival over the past 20 years.
Survival at 5 years
Globally, 50% of people who are diagnosed with mouth cancer survive for five or more years after diagnosis, this is virtually unchanged since the 1970’s.
According to Cancer Research UK, 40% of people in the UK who are diagnosed with mouth cancer, survive for five years or more after diagnosis. Overall, the five-year survival rate in Wales sits around 55% and there is little evidence of improvement, as shown below.
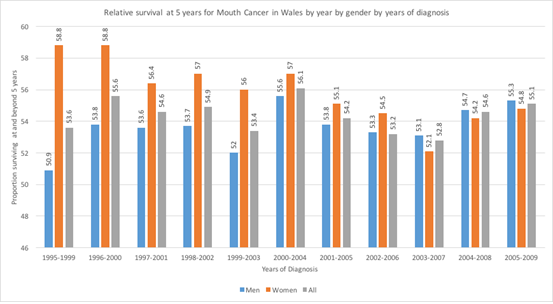
Survival can vary from 95% at five years for stage 1 mouth cancer to 5% at five years for some cancers at stage 4 disease, depending on the location of the lesion.
For people diagnosed with lip cancer, 90% survive for five or more years after diagnosis, for tongue cancer, 60% of women and 40% of men survive for five or more years after diagnosis. For mouth cancers which are not lip or tongue, 50% survive for 5 or more years after diagnosis. Reference: Cancer Research UK
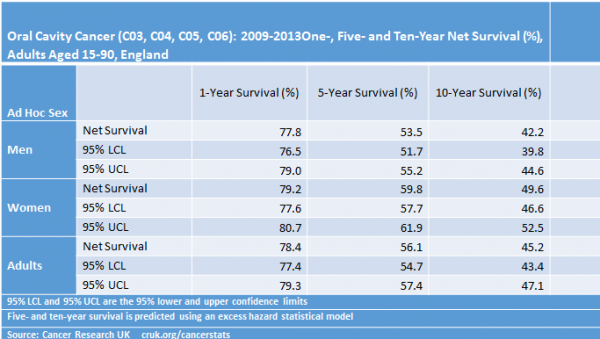
Stage of diagnosis affects survival, and people diagnosed with mouth cancer at stage 3 and 4 have a significantly reduced prognosis. Published figures vary considerably, between around 95% and 5% depending on a range of factors including site, type of cancer, stage of cancer and patient factors such as age, as demonstrated below.
| Area | Local (stage 1 and 2) % Surviving at 5 years |
Regional Spread (stage 3) % Surviving at 5 years |
Distant Spread (stage 4) % Surviving at 5 years |
|---|---|---|---|
| Lip | 93 | 48 | 52 |
| Tongue | 78 | 63 | 36 |
| Floor of Mouth | 75 | 38 | 20 |
Survival at 1 year
Survival at one year has Improved modestly in Wales and one-year survival is now 82%.
Case study
A sixty-five year old man presents to his GP.
He has a painless ulcer in the floor of his mouth under his tongue. It has been present for at least 4 weeks. He has a history of smoking 20 a day for 30 years, having quit 10 years ago.
Examination reveals a 1.2 cm ulcerated lesion, there are no cervical nodes palpable the remainder of the oral cavity is normal.
What should the GP do? 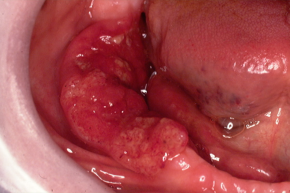
The GP tells the patient to see his dental practitioner explaining that the ulcer is potentially suspicious.
What issues does this raise?
Six months later the patient presents to the GP again. His ulcer is now painful and he has a firm 1 cm lump in his neck on the same side.
The GP referred the patient as an urgent case to the local Maxillofacial Surgery Department. A biopsy showed that the lesion was a squamous cell carcinoma. The patient needed a hemiglossectomy and a block dissection of his neck.
This case study is based on a real case in which the patient did not follow the GP’s advice. Fortunately, in this case, there are no signs of recurrent disease five years later.
Would this happen in your practice?
How could you prevent this from happening?

